By Claire Bacon, ACN, CNC
I feel like inflammation is a word we in the holistic community throw around a lot. You’ve probably heard of anti-inflammatory medication (NSAIDs) and various anti-inflammatory diets. You know that inflammation (from injury) hurts and reducing inflammation (with ice) feels better. But do you really know what inflammation is? And how is it connected to cancer?
What is Inflammation?
Inflammation is the body’s natural reaction to infection or injury. In short, it’s the body’s response to outside threats like stress, infection, or toxic chemicals. It can also result from an insufficient supply of blood to an organ or distal tissues. For the typical layman, there can be confusion about whether inflammation is healthy or harmful. The term inflammation actually refers to many different processes in the body.
When it’s Good
Inflammation can be a localized or systemic reaction from cells in our immune system and from many other body parts. For example, the cells that line our blood vessels and those that make up our skin have unique inflammatory responses: the abilities to swell, turn red, become itchy, bumpy, or tingly are all forms of inflammation. It’s a good thing because it draws your attention to the injury/exposure. And it’s good when the inflammation captures toxins or manages to control a more widespread exposure.
The swelling, redness, and warmth are signs that your immune system is sending white blood cells, immune cell-stimulating growth factors, and nutrients to the affected areas. The immune system attacks the invader with a number of reactive molecules designed to neutralize it, including hydrogen peroxide, nitric oxide and hypochlorous acid. In this sense, inflammation is a healthy and necessary function for healing. But this type of helpful inflammation is only temporary: when the infection or illness is gone, inflammation should go away as well.
When it’s Bad
In a healthy situation, inflammation serves to kickstart beneficial healing reactions. But if immune cells overreact, that inflammation can become destructive – sometimes known as a “cytokine storm.” This type of harmful, chronic inflammation can have a number of causes, including a virus or bacteria, an autoimmune disorder, sugary and fatty foods, or even the way you handle stress. Especially stress! It’s a lot more harmful than we think.
The truth is, inflammation isn’t strictly good or bad. It can be either, depending on how long the inflammation lasts. Small flare-ups of inflammation are good because it’s our immune system working to heal our bodies. But over time, chronic inflammation can be a sign of or lead to something more concerning such as Rheumatoid Arthritis, Type 2 Diabetes or even Cancer.

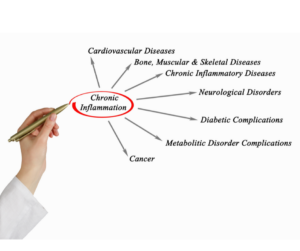
How Inflammation Connects with Cancer
Inflammation can contribute to the development of certain cancers. As many as one in five (20%) of diagnoses could find their cause in chronic inflammation. For example, there is a strong connection with bowel diseases such as Ulcerative Colitis or Crohn’s and the development of Colorectal Cancer. Some researchers are studying inflammation’s role in Lung and Breast Cancer, and also the relationships between the microbiome, the immune system and our inflammatory processes. But the connection to many other cancers is less clear.
Damaged DNA
Certain exposures and cellular insults can cause damage to our DNA. Isolated lesions have been identified that can persist in our DNA and our tissues, and resist our normal repair mechanisms involved in cellular growth and repair. If such a lesion persists, it can become mutagenic, and could initiate cancer – as in uncontrolled growth and abnormal cellular activity.
Common inflammatory conditions leading to cancer include:
| H. pylori infection can lead to gastric cancer and mucosal lymphoma | HPV infection can lead to cervical cancer, anal cancer, and penile cancer |
| Autoimmune diseases can lead to cancer of the target tissue | Hepatitis viral infection can lead to liver cancer |
| Prostatitis can lead to prostate cancer | Herpes virus (HHV-8) may cause Kaposi’s sarcoma |
| Exposure to cigarette smoke, talc, radon, or asbestos may cause lung cancer | Exposure to parabens, phthalates, and other chemicals in cosmetics may cause breast cancer |
| Exposure to talc in baby powder may cause ovarian cancer | Epstein-Barr Virus can cause certain lymphomas and cancers of the nose and throat |
| HIV infection can cause Kaposi’s sarcoma, lymphomas, and cancers of the cervix, anus, lungs, liver and throat | Certain parasitic flatworms (flukes) can cause cancers of the bile ducts of the liver and the bladder |
When these inflammatory conditions go on for years and years, cell mutation and proliferation can create an environment that promotes cancer. The so-called “perfect storm” can trigger the beginning of the disease and determine how it progresses. Various signaling pathways through enzymes are key contributors that can turn on or off these internal mutations. Therefore, identifying and treating the original inflammatory cause is very important.
Using Inflammation Purposefully in Anti-Cancer Treatments
When functioning normally, the inflammatory and immune systems inhibit the development of cancer. In a process called tumor immuno-surveillance, the body has a way to perceive and eliminate transformed cells.
Cancer-associated inflammation has effects on the ability of cancer to metastasize (or spread), and on the ability of the patient to tolerate chemotherapy. At the same time, there are certain types of inflammation that help kill tumors. For example, up and coming immunotherapies can capitalize on inflammatory processes to attack and treat cancer.

Inflammatory Blood Markers to Watch
Very Common Markers
- C-Reactive Protein (C-RP) is one of the cytokines released at the beginning of inflammation. The liver releases it into the blood, especially due to bacterial or viral infections, autoimmune diseases, and certain cancers.
- White Blood Cells (WBC) will become depleted after fighting a chronic infection or inflammatory process for a long time. WBC are produced in the bone marrow, spleen, thymus, and lymph nodes. So, an abnormal WBC count could indicate dysfunction in any of these areas.
- Erythrocyte Sedimentation Rate (ESR) measures how quickly the red blood cells settle to the bottom of a test tube. Blood from patients with excess inflammation has a faster settlement (or sedimentation) rate. ESR measures the milliliters of clear plasma above the erythrocytes at the end of one hour. This usually coincides with excess fibrinogen.
- Lactate Dehydrogenase (LDH) is an enzyme involved in cellular respiration, the process by which your body transforms glucose into energy for your cells. The LDH enzyme concentrates in your muscles, liver, kidneys and red blood cells. When body tissues experience damage, they release excess LDH. When the LDH test is high, that means certain tissues are damaged by either a chronic (long-term) or acute (short-term) disease or injury.
Less Common Markers
- CA-125 is used to monitor how well cancer treatments are working and if cancer has come back, especially in the ovaries, fallopian tubes, or peritoneum (lining of the abdominal cavity). It’s not the most accurate test, and often gives false positives or false negatives.
- Calcitonin is often checked when thyroid dysfunction or cancer is suspected.
- Plasma Viscosity (PV) measures the thickness of blood. Just like the ESR test, it checks for an increase in certain blood proteins that increase during inflammation. PV is important when diagnosing inflammation caused by bacterial infections, because it doesn’t show up in viral infections or connective tissue disease.
- Fecal Calprotectin is used to detect inflammation in the intestines. Neutrophils traveling into an inflamed gastrointestinal (GI) tract release high levels of the protein Calprotectin, which can be found in the feces.
Additional testing methods are listed here.
How to Keep Inflammation in Check
Healthy Diet
It should be obvious by now (if you have been reading our blogs) that your diet holds the key to keeping inflammation in check. The most well-known foods to lower your cancer risk are:
- Broccoli sprouts and other cruciferous vegetables for Indole-3-Carbinol
- Onions and garlic provide anti-inflammatory sulforaphanes
- Choose apples, onions, and organic tea for quercetin
- Eat wild-caught seafood and seaweed as a source of iodine
- Consume raw Brazil nuts for selenium

Daily Activities
In addition, you’ll want to watch your daily activities to lower your risk:
- Keep your vitamin D level up (sunshine is best!)
- Avoid unnecessary x-rays and mammograms (use thermography in between scans!)
- Use a good water filter; avoid unfiltered tap water
- Avoid parabens and fragrances in personal care products
- Reduce sugar in your diet as much as possible, especially high fructose corn syrup
- Clean your home with only nontoxic cleaners like vinegar and essential oils
- Utilize coffee enemas and colon hydrotherapy to promote detoxification
- Spend time in an infrared sauna or use red light therapy to increase cellular processes
- Immediately shower off pesticide residues after being on a golf course.
Helpful Supplements

- Turmeric Forte is our best systemic anti-inflammatory support, useful for almost any chronic inflammatory process. This product includes Fenugreek fiber, to hold the curcumin in the bloodstream longer to perform its beneficial actions.
- Olprima EPA/DHA contains concentrated essential fatty acids (EPA & DHA) for cell membrane and brain health. This product is more concentrated than your average anti-inflammatory fish oil.
- Multizyme contains food-sourced enzymes to work on clearing tissue debris, good for an inflamed gut, effective against intestinal parasites, too. Remember – our Standard American Diet is probably our #1 underlying factor driving inflammation!
- Black Cumin Seed Forte can enhance the liver´s detoxification enzymes and can neutralize cancer-causing free-radicals. We lovingly call it “the cure for everything but death” because it is so efficient at calming inflammation in many tissues throughout the body.
Final Thoughts
Clearly, there are a multitude of ways that inflammation can take a toll on a body. But we have just as many ways to tell inflammation, “You’re not the boss of me!” That’s right, you can take control of your health and maintain a healthy level of inflammation, just by following the steps above.
Please let us know if you need personalized help or if you have any questions!